Long-Term Patency of Double-Barrel Endovascular Stenting for Occlusive Peripheral Vascular Disease
Abstract:
“Double-Barrel Stenting,” or DBS technique, has been described in single case presentations with patency data of one year only. We present our experience with multiple patients in both the SFA and the iliac distribution, with long-term follow-up of > 5 years.
Over the past 10 years, we have employed this novel technique in situations where the vascular stent in the SFA, CFA, or iliac arteries had a chronic occlusion, with or without fracture or deformity of the existing stent, that was uncrossable with a wire and catheter.
In these situations, we have been able to cross into the subintimal space within the vessel wall, alongside the occluded stent, and reestablish a viable lumen supported by a new stent deployed alongside the occluded one. All the procedures listed were performed as outpatient, under conscious sedation. All subjects had angiographic as well as clinical success and were discharged the same day with no complications. All subjects were followed clinically and with arterial duplex ultrasound (US) at least annually. Some subjects also had angiographic follow-up.
Case #1:
History and Symptoms
A 78-year-old man presented with progressive symptoms of claudication. He was Rutherford Class 3 and had a history of extensive and bilateral peripheral vascular disease. His PAD history dated back to 2005, with the insertion of two overlapped nitinol self-expanding bare-metal stents in the right mid to distal SFA, which successfully resulted in the resolution of symptoms. Subsequently, the patient developed occlusive in-stent restenosis with recurrent lifestyle limiting claudication in 2008 that did not respond to a walking program and medical therapy.
The patient was referred for surgical consultation and was deemed to not be a good candidate for femoral popliteal (Fem-Pop) bypass surgery. The patient was already on optimal medical therapy for peripheral vascular disease. Percutaneous intervention was discussed and agreed to with the patient.
The patient’s co-morbidities were as follows:
- Extensive bilateral peripheral arterial disease
- Coronary artery disease with prior DES in LAD
- Dyslipidemia
- Hypertension
- Type 2 diabetes mellitus
- Obesity
At a five-week follow-up, the patient reported a complete resolution of claudication symptoms.
A one-year arterial doppler showed no evidence of in-stent restenosis of the double-barrel stent. Right leg ABI was 1.08.
A follow-up ultrasound at 3 years did not demonstrate any evidence of in-stent stenosis of the double-barrel stent. Recurrent symptoms at 38 months led to an arterial duplex US, which showed severe progression of disease in the ostial SFA and the popliteal but not the DBS segment.
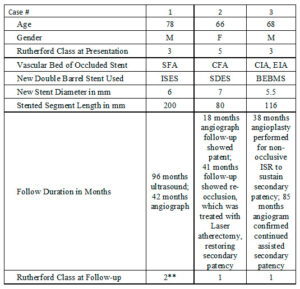
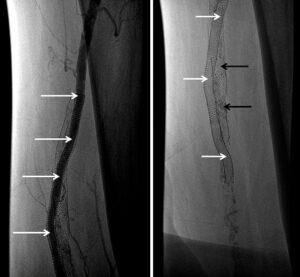
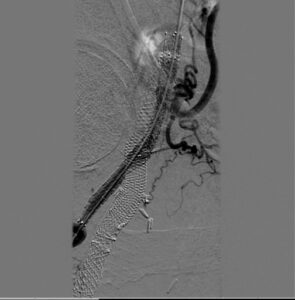
Angiography performed 3 years and 8 months following the procedure demonstrated excellent patency of the DBS (Picture). Interventions were performed at sites other than the double-barrel stent.
A Sept. 2016 US follow-up showed continued patency. The patient had no clinical symptoms of claudication.
Procedure Highlights
Access was gained in the left common femoral artery. We advanced a 7-frech Pinnacle 65cm sheath up and over to the right CFA. We were able to probe the vessel outside the previously occluded stent and gain access to the true lumen of the vessel beyond the occluded stent in the distal right SFA. A number of wires were used, including stiff Glidewire and an Amplatz wire. The stiff straight guidewire was used, along with a vertebral catheter, QuickCross catheter, and Trailblazer 0.035 catheter. We dilated the vessels with a 3.5mm Nanocross balloon. We then dilated the right superficial femoral artery with a 6mm balloon, followed by a 7mm balloon. After dilation, right SFA occlusion went from 100% to 60% severe recoil. We deployed 6×120 and 6×80 Supera stents, overlapping them with care to improve stacking of the stents to optimize radial strength. This was in the mid to distal SFA. The completion angiogram revealed a good result, with less than 20% residual stenosis at the SFA post double-barrel stenting. Patient tolerated the procedure well and was kept on DAPT.
Case #2:
History and Symptoms
A 66-year-old female presented with a history of very complex PAD. A failed right Fem-Pop bypass and multiple prior right SFA and CFA interventions, including stenting with eventual failure, led to right Above Knee Amputation (AKA). The patient had a nonhealing wound of the right leg stump and rest pain.
The patient’s co-morbidities were:
- Hypertension
- Morbid obesity
- Venous insufficiency
- Diastolic Chronic CHF
An angiogram showed patent abdominal aorta, bilateral common iliac arteries with existing stent, and occluded bilateral internal iliac arteries. The distal right external iliac artery had 60% stenosis. The left external iliac artery was patent. The right common femoral artery had an occluded stent jailing a known ostial CTO of the right profunda femoral artery, which filled poorly via collaterals. The right superficial artery was occluded.
Procedure Highlights
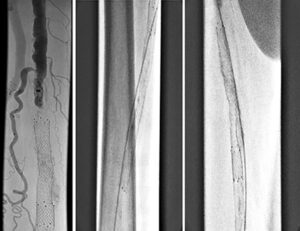
We gained left femoral artery access with up-and-over technique sheath advance to the right external iliac artery. As expected, we failed to cross the right CFA occluded stent to the jailed right profunda. Ultrasound access was obtained in the right profunda femoral artery in a retrograde fashion. We probed the chronic total occlusion of the ostial segment of the right profunda and the CFA in retrograde fashion, but we could not get into the true lumen of the right external iliac. We then used the IVUS guided crossing device, “Pioneer,” and successfully crossed the occlusion of the right common femoral artery. The entire crossing passage was outside the existing occluded CFA stent and inside the wall of the CFA. The lesion was pre-dilated with a 5×20 mm PTA balloon and then a 6×40 mm PTA balloon. Despite the good release of the lesion at 10 atm, there was severe recoil post dilation of 80% residual stenosis. We inserted a 7×80 mm Zilver PTX DES stent into the right common femoral artery, followed by a balloon expandable short stent at the iliofemoral junction for persistent recoil.
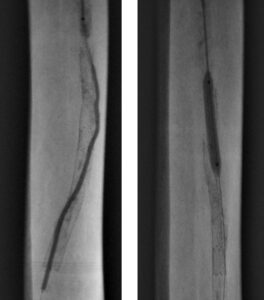
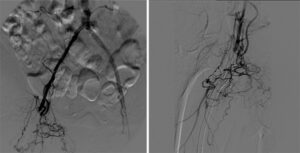
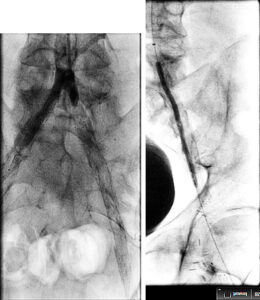
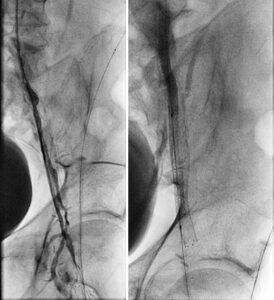
The completion angiogram showed excellent results, with the initial 100% chronic total occlusion of the common femoral artery and profunda femoral vessels reduced to under 30%, and the terminal right external iliac 60% reduced to less than 30%. The entire new stent was deployed in double-barrel fashion alongside the occluded R CFA old stent. The patient healed her nonhealing right AKA stump wound within three months post intervention. Eighteen months later, recurrent vague stump pain with suboptimal arterial duplex US led to another angiogram (Figure 8) that confirmed continued patency.
Timeline
Sept 2013: Index procedure
April 2014: Follow-up angiogram shows patent
March 2015: Follow-up angiogram shows patent
Feb 2017: Angiogram shows reocclusion; treated with Laser 1.4 followed by 6 mm PTA with good 10% passed
CASE #3:
History and Symptoms
A 68-year-old male with a long history of extensive atherosclerosis presented with left leg ischemic rest pain of a few weeks’ duration. The patient had prior remote bilateral iliac artery stenting, failed lower extremity bilateral Fem-Pop bypass and CFA endarterectomy, and remote right-to-left femoral-femoral (Fem-Fem) bypass for left iliac stent occlusion.
An angiogram showed patent aorta, as well as right common and external iliac stents. Left common iliac and left external iliac had stents and known CTO. The Fem-Fem bypass was occluded. The left CFA was also occluded with patent left profunda and occluded left SFA.
Procedure Highlights
It was a technically difficult procedure requiring 5 hours, with the first 2.5 hours spent declotting the Fem-Fem bypass without success through right femoral access.
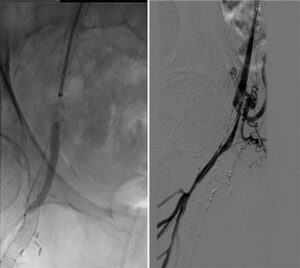
We then obtained access in the left brachial artery, with additional access in a retrograde fashion in the left profunda femoris. We successfully crossed the contiguous CTO of the left common iliac and left external iliac, as well as the left common femoral artery. The left iliac segment stent long CTO crossing would only occur outside the existing occluded stent. We conservatively carried out angioplasty of the iliac segment with progressively larger balloons to avoid vessel rupture. The patient was kept lightly sedated with frequent questioning about any pain and rigorous hemodynamic monitoring. Despite good balloon expansion, there was, as expected, severe recoil necessitating double-barrel stenting of the new lumen.
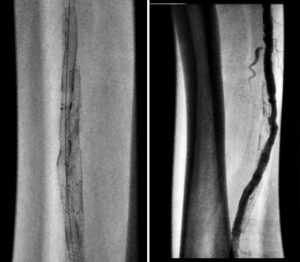
We chose bare metal stents to keep the sheath size small in the diffusely diseased brachial and profunda. We stented the left common iliac and left external iliac artery using a combination of a 6×58 Omnilink and 5×58 Omnilink, respectively, and the left CFA using an 8×80 Absolute stent covering the entire length of the vessel (CFA was de-novo stenting).
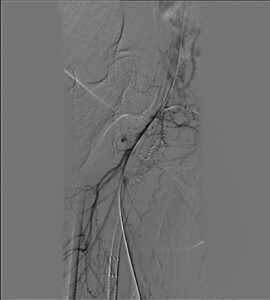
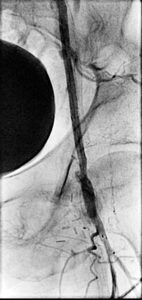
Final angiographic findings were that the left CFA, common iliac, and external iliac reduced to less than 20% with well-deployed stents. The left SFA was totally occluded with good flow into the left profunda femoris, which then collateralized at the popliteal.
The patient tolerated the procedure well and had immediate relief of his rest pain, with only claudication at a moderate distance that was not lifestyle-limiting.
Timeline
Jan. 2012: Index procedure
March 2015: Angiogram shows ISR, treated with PTA for secondary patency
April 2019: Angiogram follow-up shows patent iliac stents
At that point, the left profunda femoris sheath was removed and Mynx device deployed with good hemostasis. The left brachial sheath was removed in the holding area with good manual compression on the left brachial site with good hemostasis. The patient was kept overnight for observation and was sent home the next day with no complications.
We followed up with duplex ultrasound exams through 2019, which demonstrated the stents were still patent.
Discussion:
While subintimal double-barrel stenting has been described in the literature, there have been no reports about long-term patency.1-3
Our sample size is admittedly small yet shows durable primary and assisted patency up to 8 years. Double-barrel stenting may be an excellent option for patients who are not surgical candidates and are suffering from recurrent lifestyle-limiting claudication or CLI after the failure of previous stenting in both the iliac and femoral vessels. Our anecdotal experience suggests that the “adventitial” placement of stents did not lead to more restenosis, challenging the long-held but unproven belief that central vessel crossing is associated with better durability.
We recognize that this is a very small series of individual cases and that no conclusions can be made except for stating that double-barrel stenting seems to be a safe option to offer those patients who have uncrossable occluded stents.
- Duterloo D, Lohle P, Lampmann L. Subintimal Double-Barrel Restenting of an Occluded Primary Stented Superficial Femoral Artery. CardioVascular and Interventional Radiology. 2007;30(3):474-476.
- Ferraresi R, Ferlini M, Pomidossi G, Sozzi F, Bonanomi C, Danzi G. Side-by-side stenting technique to recanalise a complete in-stent occlusion of the superficial femoral artery. Journal of Cardiovascular Medicine. 2007;8(11):965-966.
- Nakamura A, Nakajima S, Endo H, Takahashi T, Nozaki E. Successful outside-the-stent stenting for an occluded primary stented superficial femoral artery. Cardiovascular Intervention and Therapeutics. 2013;29(2):187-192.
Banerjee S, Patel H, Sheorain V, Grover T, Parakh R. Double Barrel In Situ Recanalization of Thrombosed Nonretrievable IVC filter. Annals of Vascular Surgery. 2016;33:229.e11-229.e15.